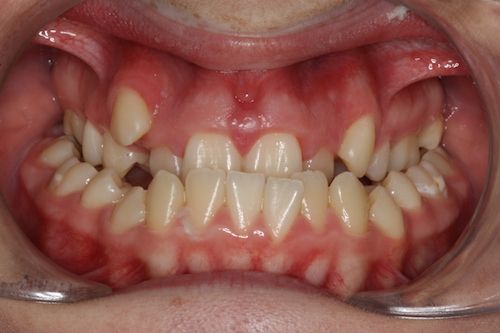
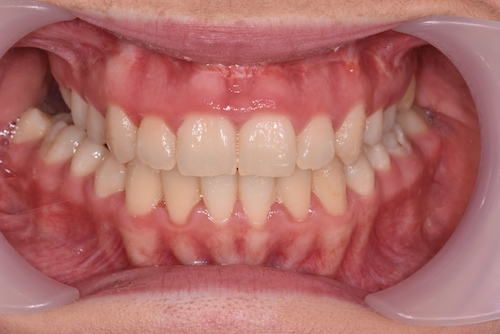
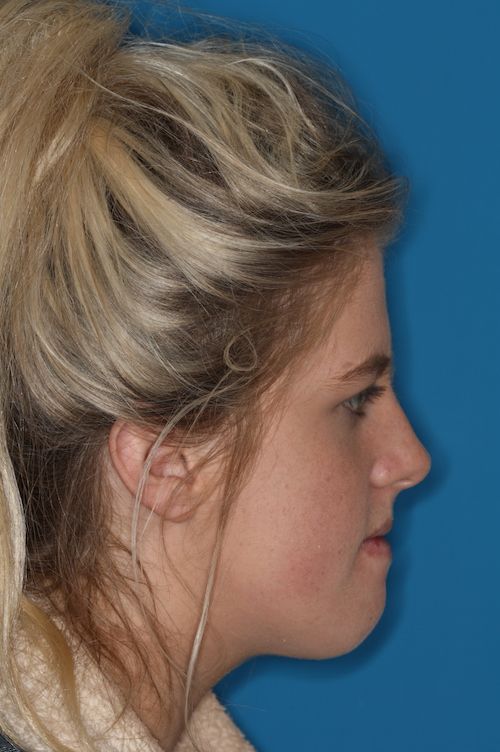
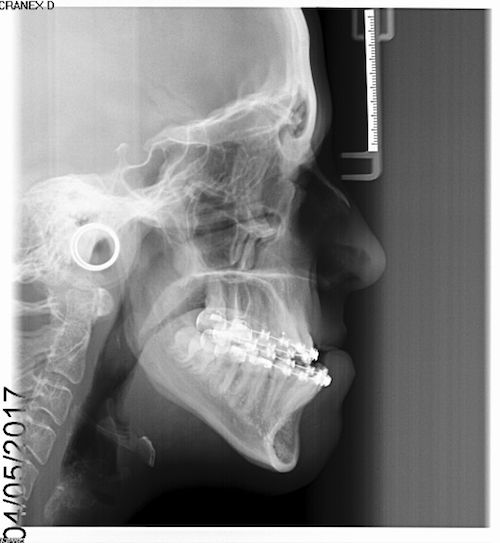
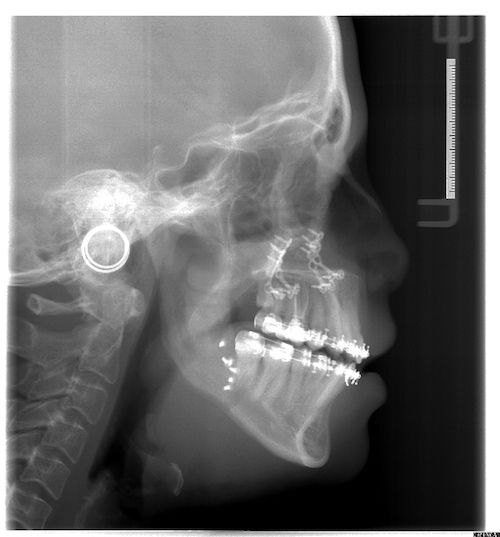
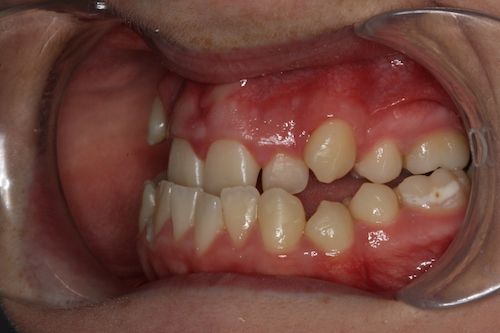
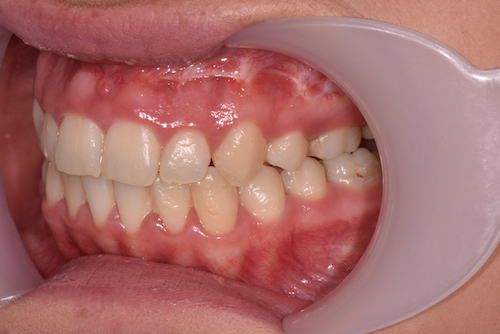
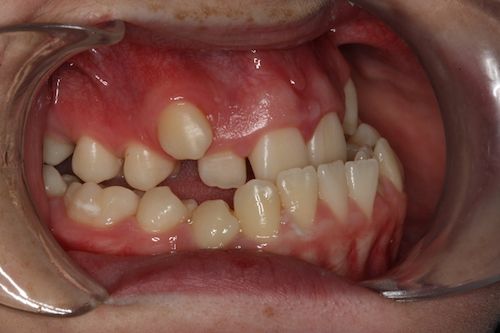
Facial Correction (Jaw Corrective Surgery)
For patients considering having Orthodontic and Jaw Corrective Surgery treatment:
Treatment Aims
When the bones of the face and jaws are out of balance with each other, orthodontics alone will often not be able to position the teeth in order to create a functional bite. This imbalance between the jaws can result in a combination of problems. These may include:
- Difficulty eating due to teeth not meeting correctly
- Compromised facial appearance
- Tooth damage/uneven wear and soft tissue trauma (ulceration, soreness)
- Crowded, irregular teeth
- Jaw joint (Temporomandibular joint – TMJ) problems
Surgery may involve either the upper jaw, lower jaw or both depending on the skeletal discrepancy of your particular case. This will allow the teeth to meet correctly and provide you with an improved bite, and often there is an accompanying improvement in your facial appearance and profile.
What are the alternatives?
Mr Duncan and his team will explain the specific options available to you at the joint clinic appointment. Doing nothing is always an option. You must not feel that surgery is the only way forward to correct a dento-facial imbalance. This surgery wasn’t readily available 50 years ago, and people have managed with their atypical bites throughout life. However, your dentist or GP who referred you to the joint clinic, feels that you MIGHT benefit from jaw corrective surgery – again all options will be discussed with you specifically with YOUR face and bite in mind. Exploring these options does not commit you to any treatment and you can change your mind at any point along the treatment pathway.
What does the treatment involve?
The treatment varies in length from case to case but usually takes between 2- 3 years to complete.
- Orthodontic treatment for approximately 18 months
- Surgery – 6 weeks recovery time
- Orthodontics after surgery for a further 6 months (fine-tuning your bite)
Why do I need orthodontic treatment as well as jaw surgery?
Your teeth need to be aligned, levelled and moved into the correct position ready for your jaw surgery to take place and remain stable after the surgery. This can often result in your bite becoming worse over the period of orthodontic treatment, but you have to remember that your teeth will be in a better, more stable position after the jaws have been moved into their correct planned position.
What does the operation involve?
This will vary according to the type of surgery that has been planned by Mr Duncan’s team. All the incisions are carried out inside the mouth apart from 2 very small 2-3mm scars in both cheeks at the angle of your jaw (only if lower jaw surgery is carried out). Prescription bone cuts are then made and your jaws are moved into their planned position relative to each other. They are then secured in position with either titanium mini plates or screws, which stay in permanently unless they become loose or infected. The soft tissues are then sutures together with dissolving stitches, which do not need to be removed, and should dissolve themselves within 3 weeks.
How long will I be in hospital?
Single jaw surgery currently involves an overnight stay, whilst bimaxillary surgery (both upper and lower jaws) will require 2 nights stay. In selective cases, single jaw surgery may be carried out as a day case procedure.
Will I have pain relief after the operation?
The Anaesthetist who will be putting you to sleep for the operation will prescribe you some pain control which you can control yourself (Patient Controlled Analgesia). This device can be pressed intermittently to allow some pain relief medication to be administered straight into your veins – but you won't necessarily get a dose of medicine every time you press the PCA pump – this is a safety feature and designed to prevent you from accidentally overdosing with strong opioid pain relief. After 24 hours, this PCA is taken down, and you will be prescribed regular codeine and paracetamol tablets to take 4 times daily. You can take ibuprofen in between these doses regularly, provided you are not asthmatic, are allergic to ibuprofen, have any stomach ulcers or any kidney problems.
Facial cooling mask - Hilotherapy
As soon as you wake up in recovery from your procedure, a facial cooling mask will be fitted which straps around your head with Velcro ties. This significantly reduces your swelling in the initial post-operative period, and we strongly recommend you keep the mask on as long as possible whilst you are in hospital. The nursing staff will teach you how to disconnect the device should you wish to go to the toilet. You do have the option of hiring the device at home for 1-2 weeks at a fee, and the team will provide you with the necessary information for this at the pre-op appointment.
What are the potential risks and side effects of surgery?
As with any surgery, there are general risks such as post-operative pain, swelling, bleeding, scars, infection risk, sutures. There are also specific risks with regards to your particular operation:
– Upper jaw surgery: temporary or permanent numbness of upper lip (full recovery is likely) , nasal tip changes, altered facial appearance, relapse, abnormal bite (malocclusion) , plate removal if screws become loose or infected
- Lower jaw surgery: temporary or permanent numbness of the lower lip or chin (8-15% cases), screw removal , malocclusion, relapse, jaw joint problems
What are the expected benefits of surgery?
- Improved facial appearance
- Improved function – better bite, no pain / trauma on biting
- Straight teeth
Will I need to have teeth extracted before surgery?
You may need multiple extractions prior to surgery – orthodontic extractions are required to make space to align teeth, ready for the surgery. Lower wisdom teeth ideally need to be removed 6-9 months prior to any lower jaw surgery, as this makes your surgery more predictable, with a more favourable outcome.
What type of brace will I need to wear?
Fixed (train-track) braces are used because they allow the most accurate positioning of the teeth prior to surgery.
Are the braces removed for the operation?
No. The braces stay in position for the operation, and Mr Gowans will add on some metal hooks just before your surgery which are needed to position your jaws only DURING the operation. You may need a further 6-9 month course of orthodontics after the operation to ‘fine-tune’ your bite.
Will I look different after the operation?
There may be some soft tissue changes in your profile afterwards, so you may look slightly different once all the swelling has subsided. Occasionally you may have some changes in the shape of your nose, if you have upper jaw surgery, and this will be discussed at the pre surgical appointments with Mr Duncan.
Are there any particular diet restrictions I need after the operation?
After the operation, you will have a more liquid diet for the first few weeks. It is important you do not bite strongly together or bite into any hard foods as this may cause the small metal plates put in your jaw to move/break, resulting in your jaws moving out of their planned position. Dietary advice will be given to you during the post-operative period.
Toothbrushing: a babies toothbrush is recommended as you will have some swelling and bruising after the operation, therefore you will have difficulty in opening your mouth. This will make toothbrushing more difficult, but you must brush the teeth you have access to, which will probably only be the front teeth initially. Brush all surfaces of the teeth in the morning and just before going to bed.
Mouthrinses: Corsodyl mouthwash will be given to you whilst you are in hospital after the operation. We advise you to continue using Corsodyl mouthrinse for at least 4 weeks after your operation at least 3-4 times daily. Do not use fluoride mouthrinses whilst using Corsodyl. You can go back to using your fluoride mouthrinse when you have finished using the Corsodyl.
Salt-water irrigation is also useful in keeping the mouth clean after surgery. This can be used in conjunction with the Corsodyl mouthwash. You will be given a 20ml syringe on the ward. Fill a cup with cooled boiled water, add a teaspoon of salt and fill the syringe. Gently flush the solution around all 4 quarters of your mouth several times a day, ideally after mealtimes to remove excess food debris.
Will I still need to see my regular dentist?
Yes. It is important that you still have regular dental check ups, as your orthodontist will not be carrying out any additional dental treatment that you may need. A clean mouth is vital in order for your wounds to fully heal, and this needs to be maintained long term especially whilst you still have braces on the teeth.
What happens next?
If you are interested in finding out more about this treatment, Mr Duncan and Mr Gowans will see you together on the joint clinic, once study models, X-rays and photographs have been carried out. They will want to know your concerns and what you hope to benefit from jaw corrective surgery. All the options will be explained at this joint clinic appointment.
If they decide you are a suitable candidate for surgery, and you decide to proceed with this pathway, you will then be given a series of orthodontic appointments for brace fitting and orthodontic treatment.
If you have any further questions you wish to ask, please write them down and bring them with you to your joint clinic appointment. It is important you fully understand what is involved before you commit to having this treatment. You can still back out of treatment at anytime along this pathway, but you will be made aware at the start, that once you have had teeth extracted for orthodontic purposes in preparation for surgery, this may affect your bite longterm, should you chose not to proceed with surgery.
Useful links:
http://www.bos.org.uk/Public-Patients/Your-Jaw-Surgery/Patient-Journey
“Since undergoing surgery, it has changed my life! What an amazing feeling it is to be able to smile. I couldn’t be happier with the outcome. I received outstanding care from start to finish by Mr Duncan and his team. I really couldn’t have asked for more.” - Emily Scott, jaw corrective surgery patient.